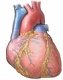
Congestive Heart Failure
in Elderly
Signs, Symptoms and Treatment
Congestive heart failure in elderly, otherwise referred to as CHF, is a condition in which the heart's function as a pump is inadequate to meet the body's needs.
It can occur when the heart is weakened or damaged from diseases or the demand for oxygen by the body is more than the heart can supply.
CHF is progressively more common with increasing age and is a serious condition. It has been reported to affect 25 percent of people older than 85 years of age.
The heart acts as a pump for blood to take oxygen and nutrients to the body. When the heart is damaged, this pump (the heart) will work less efficiently and the pumping action may not be strong enough to move enough blood around to supply enough oxygen and nutrients to the body.
This is further complicated by aging as there is a loss of muscle cells which results in the heart becoming thicker and stiffer.
People diagnosed with CHF usually have a life expectancy of 1 to 5 years though the course is extremely variable between every person. Though there is no cure for CHF, it can be managed well with lifestyle changes and treatment so many seniors return to a full life.
Congestive heart failure in elderly is diagnosed by the physician and is based on a thorough medical history, physical examination and selected laboratory tests.
Diseases that damage or weaken the heart and may increase risk of CHF include:
- Heart attacks
- Long standing high blood pressure
- High blood cholesterol
- Infection of the heart (myocarditis or endocarditis)
- Coronary artery disease
- Longstanding and/or excessive alcohol or drug abuse
- Heart valve disorders (can be too narrow or leaky)
- Diabetes
- Being obese or overweight
Diseases that demand more oxygen than the body can supply and may increase risk of congestive heart failure in elderly include:
- Hypothyroidism
- Anemia
Congestive heart failure in elderly can affect the organs of the body including:
- Kidneys which may not get enough oxygen and cannot secrete salt and water properly
- Lungs which may become congested with fluid and cause shortness of breath
- Liver may retain fluid and not be able to excrete toxins
- Intestines become less efficient absorbing nutrients and medicines
Signs and Symptoms
Signs and Symptoms of CHF:
- Fatigue
- Ability to exercise may diminish
- Swelling of ankles, legs and abdomen
- Shortness of breath; particularly when lying flat or during exercise. Seniors may be wakened in the night gasping for breath.
- Weight gain of 2-3 pounds in 1-2 days
- Bloating or feeling full all the time
- May have increased need to urinate due to more fluid in the body, particularly at night
- Nausea, abdominal pain and/or decreased appetite due to fluid in the liver/intestines
- Cold or cold symptoms that last longer than a week in conjunction with some of the above symptoms
Treatment
Treatments for seniors with CHF need to be tailored to their specific disease state and should be done on the recommendation of their physician. Some of the treatments such as heart transplant or mechanical devices may not be appropriate for people of advanced age with CFH but this can be discussed with your doctor.
Underlying heart disease combined with certain medications can worsen CHF. Review of medications and underlying disease with your loved one's physician is important.
See Elderly Medication for more tips on how to ensure your physician and pharmacist is aware of all medication interactions.
Some treatments for congestive heart failure in elderly include:
- Lifestyle modifications: Reducing sodium intake; no more than 2 grams of sodium is often recommended; Regulating fluid intake; the typical "8 glasses a day" does not apply to seniors with CHF. Fluid intake should be directed by your physician.
- Consulting a dietician or nutritionist who specializes in CHF may be advised by your physician
- Regular exercise that is tailored to the individual's tolerance and only when person is stable
- Medications to improve symptoms and prolong life
- Biventricular pacemaker may be indicated if the left and right side of the heart don't beat in rhythm
- Mechanical assist devices that are designed to do part or all of the pumping function of the heart
- Heart transplant
- Take medications regularly
- Eat a healthy diet including low sodium and carefully regulated fluid intake; eat fibre regularly
- Abstain totally from alcohol or have one drink a day at most as prescribed by your physician
- Decrease or abstain caffeine intake
- Weigh yourself daily, if you see weight gain of 2-3 pounds in 1-2 days, consult your physician immediately
- Smoking cessation
- Get plenty of sleep
- Manage stress
- Flu shot once a year
Potentially reversible underlying factors that you may discuss with your physician:
- Inadequate blood flow to the heart may be restored through coronary artery surgery or catheter procedures (angioplasty, stenting)
- Valve surgery for those who's CHF is caused by severe valve disease
- Aggressive blood pressure control when CHF is caused by longstanding, uncontrolled high blood pressure
- Abstinence from drinking if CHF is caused by chronic, severe alcohol abuse
- CHF that is caused by other diseases that may be partially or completely reversible by taking certain actions
Return to Elderly Diseases
Return to Caring for Aging Parents





New! Comments
Have your say about what you just read! Leave me a comment in the box below.